How Living Against Your Body Clock Can Compromise Your Immune System

Some people fall asleep within minutes, anywhere, in any position. Others need a carefully constructed evening routine, the right temperature, the right level of quiet, and still end up lying awake for hours. It is easy to assume that the first group has nothing to worry about when it comes to sleep.

Some people fall asleep within minutes, anywhere, in any position. Others need a carefully constructed evening routine, the right temperature, the right level of quiet, and still end up lying awake for hours. It is easy to assume that the first group has nothing to worry about when it comes to sleep.
But how quickly you fall asleep is only one part of the picture. While a meaningful indicator of sleep quality, it is separate from the question of whether your body clock is running on the right schedule.
Someone who sleeps well Monday through Friday but stays up two or three hours later on weekends is sending their biology a different signal every week. So is someone who eats dinner at 7 PM on some days and 11 PM on others, or who gets bright light exposure late at night from screens. The immune system, metabolism, and hormones are all governed by a 24-hour internal clock that depends on consistent signals to function properly. When those signals become unpredictable, the clock loses its rhythm.
That internal conflict is what researchers call circadian disruption. And its effects on immune aging run deeper than most people realize.
How your internal clock actually works
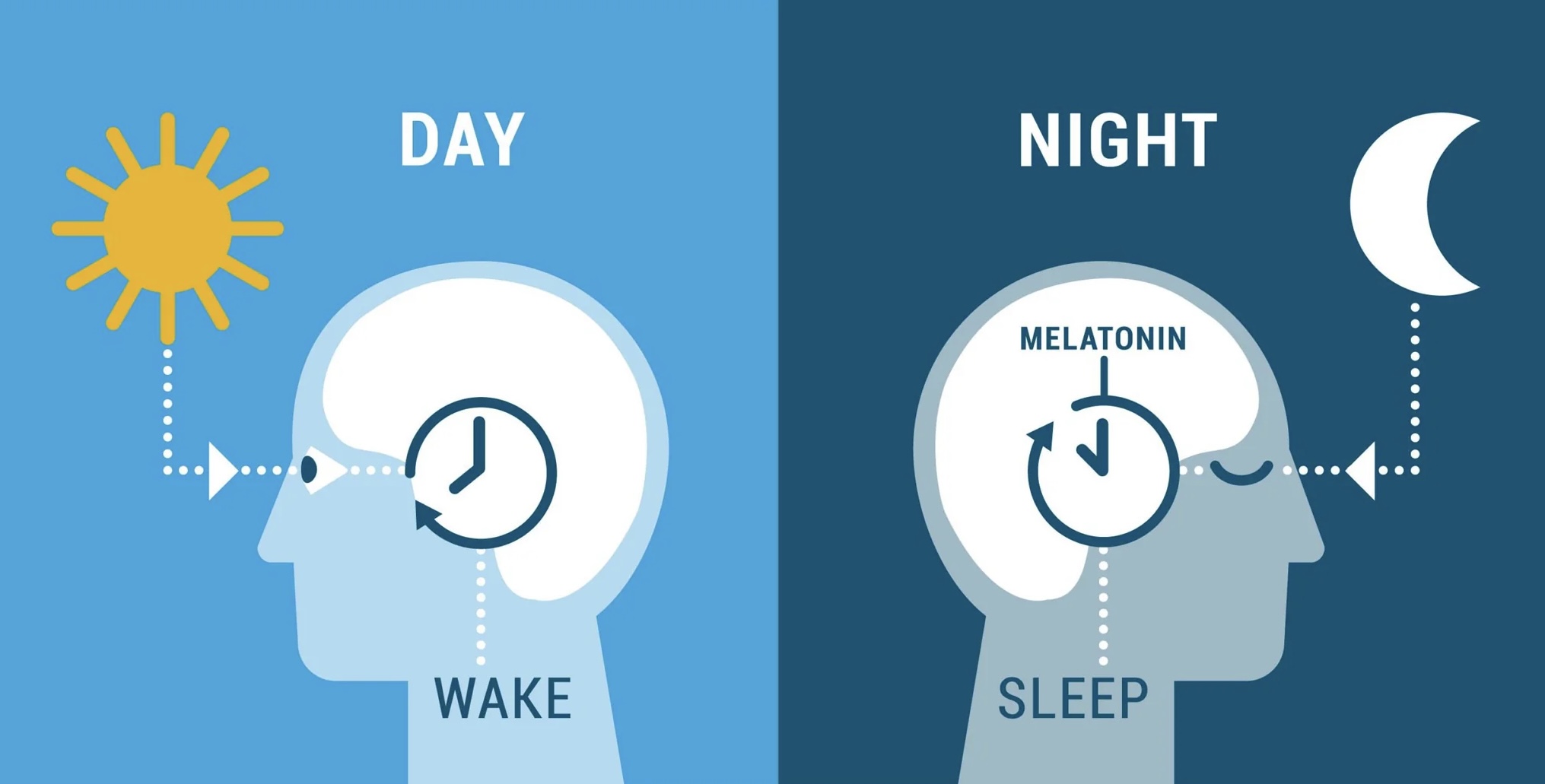
Your body runs a 24-hour biological program. The master clock sits in a small region of the brain called the suprachiasmatic nucleus (SCN), and it coordinates peripheral clocks distributed across virtually every organ and cell type: the liver, the heart, skeletal muscle, and immune cells. These clocks collectively regulate metabolism, immune activity, hormone release, and cellular repair in rhythms that repeat every single day (Roenneberg and Merrow).
The SCN is set primarily by light and darkness. But the peripheral clocks also respond to meal timing and physical activity, which means the whole system depends on multiple behavioral cues arriving in the right sequence (Roenneberg and Merrow). A late meal, a bright screen before bed, a weekend that pushes everything back by two hours. Each of these sends a signal. When those signals contradict each other often enough, the clocks fall out of sync with one another and with the outside world.
What happens next is not just poor sleep. At the molecular level, misalignment interferes with two core clock proteins, BMAL1 and CLOCK, which act as the molecular switches that control immune cell activity throughout the day (Scheiermann et al.). Under normal conditions, the immune system cycles between a daytime phase oriented toward threat detection and an overnight phase focused on resolution and tissue repair. Disrupt the clock long enough, and that cycle breaks down, which leads to the immune system getting stuck in a state of persistent low-grade activation, producing inflammatory mediators (Scheiermann et al.). This is one of the key mechanisms through which circadian disruption accelerates biological aging, and it produces no obvious symptoms while it is happening.
How widespread is circadian disruption?
More widespread than most people realize, and the numbers are worth pausing on.
Around 15 to 25% of the global workforce does shift work, putting hundreds of millions of people in direct conflict with the natural day-night cycle (Straif et al.). But the problem extends well beyond that. Over 80% of people in industrialized countries live in areas with significant light pollution, meaning genuine darkness at night has quietly become the exception rather than the rule (Windred et al., "Personal Light"). An estimated 70% of adults in developed countries have some degree of social jet lag, the mismatch between their weekday and weekend sleep schedules (Roenneberg et al., "Social Jetlag"). And the majority of people spend their evenings under blue-enriched light from phones and screens, which suppresses melatonin and weakens the circadian signal the body depends on (Dibner et al.).
Using your phone before bed or sleeping in on weekends might seem harmless in isolation. But these are not isolated habits. They are part of a pattern that has measurable consequences for long-term health.
Circadian disruption is associated with increased risk of cardiovascular disease, metabolic dysfunction, obesity, depression, cognitive decline, and cancer (Morris et al.; Erren et al.). And here is the part that tends to get overlooked: many of these risks are not simply a consequence of not sleeping enough. The timing misalignment drives them independently.
In other words, eight hours of sleep at inconsistent times is not the same as eight hours at a stable schedule. The disruption to timing has its own risks, independent of how long you sleep.
The cost of a regular schedule
Most people have never heard that shift work is classified as a probable carcinogen. In 2007, the International Agency for Research on Cancer placed it in the same category as UV radiation, based on what chronic circadian disruption does to the body over time (Straif et al.; IARC Monographs). When you hear shift work, you probably think of night shifts. But the same biological disruption can develop in people who have never worked a single night in their lives.
Think about senior executives and consultants who travel several times a month internationally and rarely allow themselves enough time to re-synchronize between trips. They probably would not describe themselves as shift workers. But the biology does not make that distinction.
Research from the Cleveland Family Study, which followed 587 adults, found that those with two or more hours of difference between their weekday and weekend sleep schedules had measurably higher levels of inflammatory markers in their blood (Girtman et al.). Later sleep timing was also independently linked to elevated inflammation, regardless of how many hours of sleep those people were getting.
What circadian disruption actually does to your immune system: a case study
A 61-year-old former nurse, with more than 30 years of career, including decades of rotating shifts, came in for GlycanAge testing ten years after retiring.
By the time of the test, her lifestyle was genuinely good. Mediterranean diet, regular exercise, and consistent sleep timing. She was also on hormone replacement therapy, which typically shifts the glycan profile in an anti-inflammatory direction and lowers GlycanAge. There was nothing in her current habits that should have flagged a problem.
Her glycan profile disagreed. Biological age was elevated. Glycan Youth and Glycan Shield, the structures associated with immune protection and tolerance, were low. Glycan Mature, associated with pro-inflammatory activity, was high. Cardiovascular, metabolic, autoimmune, and respiratory domains all came back slightly out of range. It looked like the immune system was still under the impact of years of circadian disruption, even though she had stopped working as a nurse a decade ago.
Sleep duration vs sleep timing: which one is more important
There's a widespread assumption that what circadian disruption does to your health is essentially what sleep deprivation does to your health. The research says otherwise.
Under normal conditions, the immune system follows a daily rhythm. It ramps up during the day to detect and respond to threats, then shifts into a recovery mode overnight to repair tissue and resolve inflammation. When the circadian system is chronically disrupted, that rhythm breaks down. The immune system loses its cue to switch off and instead stays in a state of low-grade, persistent activation, continuously producing inflammatory signals even when there is nothing to fight (Scheiermann et al.; Man et al.).
This type of inflammation produces no obvious symptoms. But it is exactly what researchers have identified as one of the primary drivers of biological aging.
And the evidence is clear that timing is the cause, not sleep loss. When researchers compared two groups of mice losing the same amount of sleep, the ones whose light-dark cycle was disrupted to simulate shift work developed measurable inflammatory changes. The group that simply slept less, with no timing disruption, did not (Brager et al.). In human studies, just three days of an inverted sleep schedule were enough to produce measurable increases in inflammatory markers, with nothing else changing (Morris et al.).
How to realign your life with your internal clock
Circadian-driven immune aging can be reversed, but it takes time. Months to years, not weeks. Here are some science-backed tips:
Light exposure: Get outside within an hour of waking for at least 10 to 30 minutes. This is one of the most powerful signals you can send your body clock. After sunset, dim the lights and reduce screen exposure for two to three hours before bed. Sleep in genuine darkness, blackout curtains, and no LED sources in the bedroom.
Sleep timing: A fixed wake time kept within a 30-minute window, seven days a week, is one of the most effective ways to stabilize the circadian system (Roenneberg et al., "Social Jetlag"). If you have significant social jet lag, shifting your weekend schedule back by 30 minutes every couple of weeks is a manageable way to close the gap gradually.
Consistent meal times: Your body clock responds to meal timing as much as it responds to light. Keeping your eating within a 10 to 12-hour window during daylight hours, with the first meal within 1 to 2 hours of waking and the last meal at least 3 hours before bed, reinforces the body's internal timing and supports the overnight repair processes that depend on a proper fasting window (Panda).
What you eat: A Mediterranean dietary pattern supports the anti-inflammatory glycan structures that decline with circadian disruption. Omega-3 supplementation at 1 to 2 g of EPA/DHA daily has been shown to reduce pro-inflammatory glycan modifications, with a small but measurable reduction in biological age (Yokoi-Shimizu et al.).
Supplemental support
For those who need additional help, the options with the clearest evidence include:
Low-dose melatonin at 0.3 to 1 mg, taken three to five hours before your usual sleep time. It works by shifting the clock rather than simply sedating you, which makes it a fundamentally different tool from a standard sleep aid (Lewy et al.; Herxheimer and Petrie).
Magnesium glycinate or L-threonate at 200 to 500 mg, one to two hours before bed, for sleep quality and cortisol modulation (Schuster et al.; Hausenblas et al.).
Glycine at 3 to 5 g before bed, which lowers core body temperature and has been shown in controlled trials to improve sleep quality (Inagawa et al.; Bannai and Kawai).
L-theanine at 100 to 200 mg in the evening, for those whose main obstacle is an overactive mind or nervous system before sleep (Cotter et al.).
Tart cherry extract, which combines natural melatonin and polyphenols, has been shown to improve sleep duration and efficiency (Howatson et al.).
Apigenin from standardized chamomile extract, for mild sedation without dependency risk (Zick et al.).
Bottom line
Chances are, most of us have some degree of circadian misalignment. Between 24/7 access to phones, later nights on weekends, and that Monday morning alarm that never gets easier, the conditions for a disrupted internal clock are built into modern life.
What starts as circadian disruption can silently shift the immune system toward an older, more inflammatory state long before any symptoms appear.
If you want to understand how your lifestyle is affecting the way you are aging, a GlycanAge test can measure your inflammation levels, and our team will provide you with a personalized plan on how to realign your biology and protect your long-term health.
References
Bannai, M., and N. Kawai. "Glycine Improves the Quality of Sleep." Journal of Pharmacological Sciences, vol. 118, no. 2, 2012, pp. 145–148. https://doi.org/10.1254/jphs.11R04FM
Brager, A. J., et al. "Sleep Loss and the Inflammatory Response in Mice Under Chronic Environmental Circadian Disruption." PLoS ONE, vol. 8, no. 5, 2013, e63752. https://doi.org/10.1371/journal.pone.0063752
Cotter, J., et al. "L-Theanine and Sleep: Systematic Review." Nutritional Neuroscience, vol. 29, no. 2, 2026, pp. 224–238. https://doi.org/10.1080/1028415X.2025.2556925
Dibner, C., et al. "The Mammalian Circadian Timing System: Organization and Coordination of Central and Peripheral Clocks." Annual Review of Physiology, vol. 72, 2010, pp. 517–549. https://doi.org/10.1146/annurev-physiol-021909-135821
Erren, T. C., et al. "Shift Work and Cancer: The Evidence and the Challenge." Deutsches Ärzteblatt International, vol. 107, no. 38, 2010, pp. 657–662. https://doi.org/10.3238/arztebl.2010.0657
Girtman, K. L., et al. "Later Sleep Timing and Social Jetlag Are Related to Increased Inflammation in a Population with a High Proportion of OSA: Findings from the Cleveland Family Study." Journal of Clinical Sleep Medicine, vol. 18, no. 9, 2022, pp. 2179–2187. https://doi.org/10.5664/jcsm.10056
Hausenblas, H. A., et al. "Magnesium L-Threonate Improves Sleep Quality." Sleep Medicine: X, vol. 8, 2024, 100121. https://doi.org/10.1016/j.sleepx.2024.100121
Herxheimer, A., and K. J. Petrie. "Melatonin for the Prevention and Treatment of Jet Lag." Cochrane Database of Systematic Reviews, no. 2, 2002, CD001520. https://doi.org/10.1002/14651858.CD001520
Howatson, G., et al. "Tart Cherry Juice and Sleep Quality." European Journal of Nutrition, vol. 51, no. 8, 2012, pp. 909–916. https://doi.org/10.1007/s00394-011-0263-7
IARC Monographs Volume 124 Group. "Carcinogenicity of Night Shift Work." The Lancet Oncology, vol. 20, no. 8, 2019, pp. 1058–1059. https://doi.org/10.1016/S1470-2045(19)30455-3
Inagawa, K., et al. "Glycine Ingestion before Bedtime Improves Sleep Quality." Sleep and Biological Rhythms, vol. 4, no. 1, 2007, pp. 1–7. https://doi.org/10.1111/j.1479-8425.2006.00193.x
Krištić, J., et al. "Glycans Are a Novel Biomarker of Chronological and Biological Age." Journals of Gerontology: Series A, vol. 69, no. 7, 2014, pp. 779–789. https://doi.org/10.1093/gerona/glt190
Lewy, A. J., et al. "Melatonin Shifts Human Circadian Rhythms according to a Phase-Response Curve." Chronobiology International, vol. 9, no. 5, 1992, pp. 380–392. https://doi.org/10.3109/07420529209064550
Man, K., et al. "Immunity around the Clock." Science, vol. 354, no. 6311, 2016, pp. 434–439. https://doi.org/10.1126/science.aah4966
Morris, C. J., et al. "Circadian Misalignment Increases Cardiovascular Disease Risk Factors in Humans." Proceedings of the National Academy of Sciences USA, vol. 113, no. 10, 2016, pp. E1402–E1411. https://doi.org/10.1073/pnas.1516953113
Noordam, R., et al. "Associations of Outdoor Temperature, Bright Sunlight, and Cardiometabolic Traits in Two European Population-Based Cohorts." Journal of Clinical Endocrinology & Metabolism, vol. 104, no. 7, 2019, pp. 2903–2910. https://doi.org/10.1210/jc.2018-02532
Panda, S. "Circadian Physiology of Metabolism." Science, vol. 354, no. 6315, 2016, pp. 1008–1015. https://doi.org/10.1126/science.aah4967
Plećaš, D., et al. "Not-So-Sweet Dreams: Plasma and IgG N-Glycome in the Severe Form of the Obstructive Sleep Apnea." Biomolecules, vol. 13, no. 6, 2023, 880. https://doi.org/10.3390/biom13060880
Rajaratnam, S. M. W., et al. "Melatonin Phase-Shifts Human Circadian Rhythms." Journal of Clinical Endocrinology & Metabolism, vol. 88, no. 9, 2003, pp. 4303–4309. https://doi.org/10.1210/jc.2003-030460
Roenneberg, T., et al. "Social Jetlag and Obesity." Current Biology, vol. 22, no. 10, 2012, pp. 939–943. https://doi.org/10.1016/j.cub.2012.03.038
Roenneberg, T., and M. Merrow. "The Circadian Clock and Human Health." Current Biology, vol. 26, no. 10, 2016, pp. R432–R443. https://doi.org/10.1016/j.cub.2016.03.011
Scheiermann, C., et al. "Circadian Control of the Immune System." Nature Reviews Immunology, vol. 13, no. 3, 2013, pp. 190–198. https://doi.org/10.1038/nri3386
Schuster, J., et al. "Magnesium Bisglycinate Supplementation in Healthy Adults Reporting Poor Sleep." Nature and Science of Sleep, vol. 17, 2025, pp. 2027–2040. https://doi.org/10.2147/NSS.S524348
Straif, K., et al. "Carcinogenicity of Shift-Work, Painting, and Fire-Fighting." The Lancet Oncology, vol. 8, no. 12, 2007, pp. 1065–1066. https://doi.org/10.1016/S1470-2045(07)70373-X
Windred, D. P., et al. "Light Exposure at Night and Cardiovascular Disease Incidence." JAMA Network Open, vol. 8, no. 10, 2025, e2539031. https://doi.org/10.1001/jamanetworkopen.2025.39031
Windred, D. P., et al. "Personal Light Exposure Patterns and Mortality: A Prospective Cohort Study of 88,905 UK Biobank Participants." Proceedings of the National Academy of Sciences USA, vol. 121, no. 43, 2024, e2405924121. https://doi.org/10.1073/pnas.2405924121
Wittmann, M., et al. "Social Jetlag: Misalignment of Biological and Social Time." Chronobiology International, vol. 23, no. 1–2, 2006, pp. 497–509. https://doi.org/10.1080/07420520500545979
Wong, P. M., et al. "Social Jetlag, Chronotype, and Cardiometabolic Risk." Journal of Clinical Endocrinology & Metabolism, vol. 100, no. 12, 2015, pp. 4612–4620. https://doi.org/10.1210/jc.2015-2923
Yokoi-Shimizu, K., et al. "DHA/EPA Supplementation and Sleep Quality." Nutrients, vol. 14, no. 19, 2022, 4136. https://doi.org/10.3390/nu14194136
Zick, S. M., et al. "Chamomile Extract for Insomnia." BMC Complementary and Alternative Medicine, vol. 11, 2011, 78. https://doi.org/10.1186/1472-6882-11-78

Turn health content into action
Explore how biological age testing reflects immune health and inflammaging, GlycanAge for personal wellness tracking, and how to order a GlycanAge biological age test.

The Future of Healthcare is Preventative, Personalised, and Powered by Glycans
Whether you’re improving your own health, supporting patients, or driving research, GlycanAge helps you turn science into action.

How Insulin Resistance Can Accelerate Aging Before Diabetes Ever Appears
When most people hear "insulin resistance", chances are their mind goes straight to a scary place: diabetes. And that makes sense, because that's almost always the context it appears in. But framing insulin resistance purely as a diabetes risk misses something important: long before it ever becomes diabetes, insulin r…
March 23, 2026
10 minutes

Vitamin D3's Role in Chronic Disease Prevention
Discover the power of the sun! AKA.. vitamin D3.
March 4, 2025
15 minutes